A Primary Care Physician at the Heart of COVID-19
By Dr Pallavi Prathivadi
I had planned to move to Stanford in the first week of June as a Fulbright Scholar. April and May 2020 were meant to be full of goodbye parties, comparing shipping rates, and packing up my life in Melbourne to spend a year undertaking my PhD with a terrific team at the Stanford School of Medicine.
Instead, I have postponed my trip, and written an Advanced Care Plan for myself if I end up critically unwell with coronavirus.

I am preparing for surge workforce and being called in to help at the local hospital. I’ve stopped hugging my family and I am back wearing scrubs to reduce the risk of carrying contaminated clothes into my house. For my 31st birthday last week, my friend Sarah, an anaesthetics registrar, gave me a brand-new reusable P95 respirator with filters. Was there ever a time I thought a gift like that would have moved me to tears? No.
I have worked in the same clinic for 3 years now; it’s small and wonderful. I know all of the families of the staff and often immunise their kids. We have four nurses; Brooke is in her third trimester of pregnancy with a toddler at home and is still working. Winnie is a breastfeeding mother, intermittently expressing between patients and is still working. Cindy got married last weekend and is still working (no honeymoon). Emily is trying to manage the schoolwork of her two kids while they are at home and is still working. All of our doctors, nurses and receptionists have chosen to keep working as normal during the pandemic, knowingly placing themselves at risk.
It’s been reported that 10% of covid-19 positive people in Victoria (where I live) are healthcare workers- but we are not simply statistics. We are also people with families and lives, and without adequate personal protective equipment (PPE) and with increasing rates of covid-19, the wonderful nurses you have just read about are at risk. You might have followed the backlash on social media when this point is sometimes made about a healthcare worker; that we are choosing to place ourselves at risk. That no-one is forcing us to see patients. That is true, but do you honestly expect most doctors and nurses will bail during a pandemic and deny care to patients? We are here to help. And in return we are all begging help from you; conserve PPE for those who need it most and stay home.

We are trying to move to telehealth to reduce face-to-face contact with patients. I never learnt about telehealth in medical school. I am learning it now, as a consultant specialist GP in metropolitan Melbourne. Our rural colleagues have far more experience and are providing the world with very useful advice. I’m sorry we needed a pandemic to widely embrace telehealth; video and telephone consultations with doctors help thousands more patients access healthcare in a timely manner.
The difficulty I am experiencing is when I have finished taking a history, and I need to examine the patient. Easy in real life; hard via telehealth. Many people have blood pressure machines and thermometers at home and can provide their own vital signs to me over the phone. None of my patients yet have had oximeters at home, so I haven’t been able to get an oxygen saturation level. We try to manage as best as we can. Sore throat? Can you try and look in the mirror and tell me if you see pus on your tonsils? Red swollen knee? Can you copy the movements I am doing so I can see your knee’s range of movement over the screen?
Here’s where it gets harder; the baby that the first-time mum thinks has been ‘feeling hot’ but has been swaddled in several layers because it is cold and raining outside. OK, parents don’t have a thermometer at home. I can’t tell if the baby has a fever or not. If there is a fever, is it 37.8 degrees and low grade, or is it closer to 41 degrees?
What about this one: preteen has abdominal pain. OK. Parents not fluent in English but they sound worried. He’s quiet and not particularly chatty — is he just shy or is this unusual behaviour for him? How do I organise a telephone interpreter, and how can this patient be examined?
It’s easier with an obviously unwell person (send them to an emergency department). Someone with epidemiological and clinical criteria warranting covid-19 testing- also straightforward (send them to a testing centre). The 20-year-old woman with epilepsy whom I have been looking after for years and know very well- I can do this appointment via telephone no problem and fax these scripts to the pharmacy. In our medical training, our teachers tell us that 70-80% of the diagnosis can be made from the history alone and encourage us to develop superb history-taking skills. I think we generally do pretty well, and we can sort out most problems using telehealth, but not being able to examine patients is hard. What do I do about the kids in the situation above?
The 25-year-old woman for whom I was supposed to insert an Implanon contraceptive device- what do I do now? Can I trust you’ve been staying at home and have minimal coronavirus exposure for us to bring you into the clinic for your procedure? What if our inadequate PPE means you come in healthy, and then we unwittingly pass on coronavirus to you while we are still asymptomatic? Do we do what’s safer for everyone and postpone, although that may place you at risk of unintended pregnancy?
How long do we postpone immunisations, breast cancer screening, diabetes risk assessment, check of iron levels post iron transfusion, or review of a suspicious skin lesion? For how long do we put off all of these ‘non-urgent’ bread-and-butter general practice issues? For how many months do we prioritise urgent care and put preventative health on the backburner? We are short on PPE and may need to conserve it for the coming weeks if disaster strikes. So, can I justify using our very limited PPE to perform a ‘non-urgent’ cervical screening test? Should I not be saving my precious N95 respirator filters if the nightmare scenario happens and I am called in to help run a coronavirus ward at the hospital?
So many questions. It must be frustrating for you to read this article — I have not neatly provided solutions for each problem that I point out. I have offered no happy updates on what happened to the patients above, just described their uncertain clinical scenarios. We are all figuring this out as we go. Our clinic is debriefing every night to review how we performed that day. Perhaps we need to make changes to our clinic protocols for tomorrow. Perhaps a doctor has developed a mild runny nose that evening- she now has to self-isolate and be tested for coronavirus- and we will have to scramble to cover her patient lists for the next 4-5 days at least.

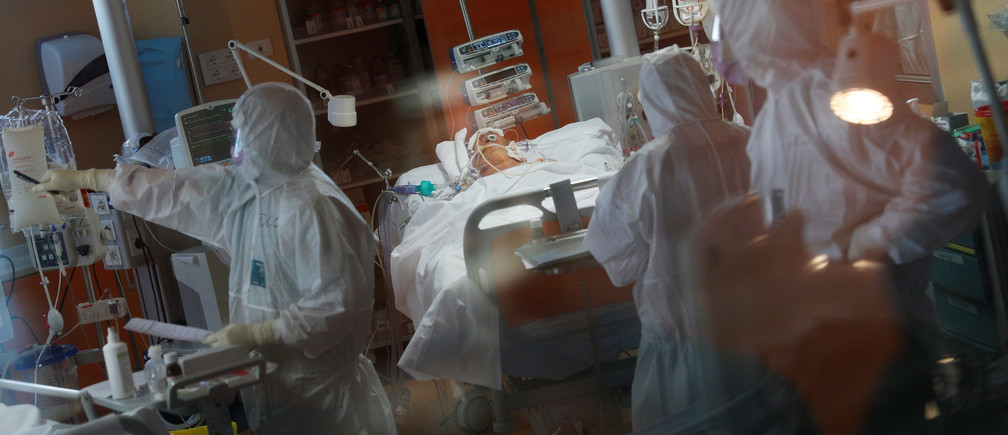
PPE is in high demand and short supply across the globe — it is exceptionally important for medical staff in ICU wards
Here’s what’s been happening with examinations- if we are worried during the telehealth consultation, we’ve been asking patients to come in face-to-face so we can properly look in their mouth, feel their abdomen or listen to their chest. We wear gloves, scrubs and a surgical mask, and use a single examination room (which our nurses will thoroughly clean after each use). We hope (we desperately hope) the patient is not in the incubation phase of coronavirus and placing everyone at risk. We are trying to get into the mindset of ‘assume everybody has coronavirus’ and take the appropriate measures to protect ourselves and other patients.
If we can avoid seeing you, we will. But if we’re worried and we need to examine you, or you need face-to-face care, we will place ourselves at risk to do what is needed. I am not an epidemiologist and I have never worked in public health. I know very little about covid-19 prediction models or virology. My PhD is about opioid prescribing in general practice. I am just a GP, but like most of my medical colleagues, I can see that this pandemic is going to need all-hands-on-deck and so I am choosing to stay and help. I guess we’ll see what happens.
Copyright © 2021 – Fulbright


 Facebook
Facebook Twitter
Twitter Linkedin
Linkedin Instagram
Instagram